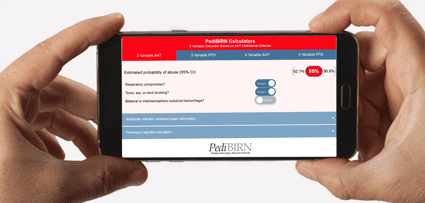
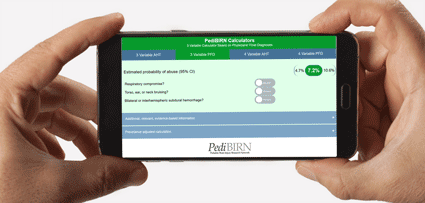
- 3 Variable Calculator Applying AHT Definitional Criteria
- Estimated probability of abuse based on:
1. Respiratory Compromise
2. Torso, ear, or neck bruising
3. Bilateral or interhemispheric subdural hemorrhage
Evidence-based Medical Screening for Pediatric Abusive Head Trauma (AHT)
To minimize missed cases, Pediatric Brain Injury Research Network (PediBIRN) investigators developed two effective AHT screening tools. Both were designed to inform physicians’ decisions to launch or forego abuse evaluations in their acutely head-injured patients under three years of age. Both are highly sensitive (≥93%), evidence-based, and simple to apply. Physicians simply confirm the presence or absence of 3 or 4 specific findings, and prospective data regarding 973 young, acutely head-injured patients hospitalized for intensive care across 18 sites does the rest!

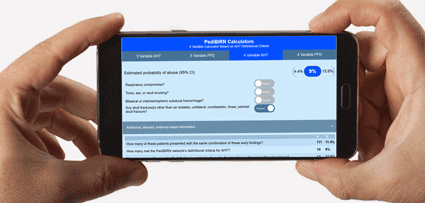
The "PediBIRN-4" identifies young, acutely head-injured patients hospitalized for intensive care who are at "higher risk" and recommends that they be thoroughly evaluated for abuse. Applied accurately and consistently, it "casts a wide net", categorizing ≥96% of AHT patients as higher risk.3,4 Its AHT screening sensitivity has been externally validated in multiple clinical settings.5,6 In a recent cluster randomized trial, PedBIRN-4 application reduced potential cases of missed AHT.7
The "PediBIRN-3" is a simplified AHT screening tool based solely on the PediBIRN 4’s first three predictor variables.8 Applied accurately and consistently, it "casts a smaller net more accurately", categorizing ≥93% of AHT patients as higher risk, but recommending fewer evaluations of patients with non-AHT. Preliminary evidence suggests the PediBIRN-3 is more acceptable to physicians, and is better suited for application in pediatric ED settings.5,8
Both screening tools can also be applied as "AHT probability calculators" that facilitate patient-specific estimation of abuse probability highly predictive (Pearson’s R ≥.91) of the overall positive yield of patients’ subsequent, completed, abuse evaluations.
Click here to compare and contrast their AHT screening performances.
Click here to compare and contrast their AHT prediction performances.
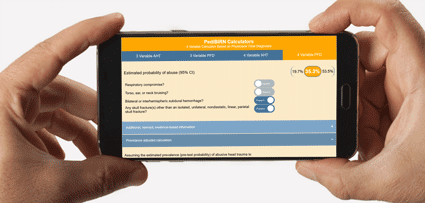
To estimate the probability of AHT after abuse evaluation, PediBIRN investigators derived and validated the "PediBIRN-7"—an evidence-based tool that incorporates the (positive or negative) predictive contributions of patients’ completed skeletal surveys and retinal exams.9,10 The PediBIRN-7's patient-specific estimates of AHT probability and likelihood ratios can be downloaded here. ![]()
Selected References:
1 Jenny C., Hymel KP, Ritzen A, et al. Reinert, S.E., & Hay, T.C. (1999). An analysis of missed cases of abusive head trauma. JAMA 1999;281:621-626.
2Letson MM, Cooper JN, Deans KJ, et al. Prior opportunities to identify abuse in children with abusive head trauma. Child Abuse Negl 2016;60:36-45.
3 Hymel KP, Willson DF, Boos SC, et al. Derivation of a clinical prediction rule for pediatric abusive head trauma. Pediatr Crit Care Med 2013;14(2):210-220. DOI:10.1097/PCC.0b013e3182712b09
4 Hymel KP, Armijo-Garcia V, Foster R, et al. Validation of a clinical prediction rule for pediatric abusive head trauma. Pediatrics 2014;134(6):e1537-1544. DOI:10.1542/peds.2014-1329
5 Hymel KP, Fingarson AK, Pierce MC, et al. External validation of the PediBIRN screening tool for abusive head trauma in pediatric emergency department settings. Pediatr Emerg Care 2022;38:269-272. DOI: 10.1097/PEC.0000000000002670
6 Pfeiffer H, Smith A, Kemp AM, et al. External validation of the PediBIRN clinical prediction rule for abusive head trauma. Pediatrics 2018;141:e20173674. DOI: 10.1542/peds.2017-3674
7 Hymel KP, Armijo-Garcia V, Musick M, et al. A cluster randomized trial to reduce missed abusive head trauma in pediatric intensive care settings. J Pediatr 2021:236;260-268. DOI: 10.1016/j.jpeds.2021.03.055
8 Hymel KP, Karst W, Marinello M, et al. Screening for pediatric abusive head trauma: Are three variables enough? Child Abuse Negl 2022:125;105518. DOI: 10.1016/j.chiabu.2022.105518
9 Hymel KP, Ming Wang, Vernon M. Chinchilli, Wouter A. Karst, Douglas F. Willson, Mark S. Dias, Bruce E. Herman, Christopher L.Carroll, Suzanne B. Haney, Reena Isaac. Estimating the probability of abusive head trauma after abuse evaluation. Child Abuse & Neglect, 2019;88:266-274.
DOI: 10.1016/j.chiabu.2018.11.015
10Kent P. Hymel , Christopher L. Carroll , Terra N. Frazier, Kerri Weeks, Bruce E. Herman, Mark Marinello, Yiming Chen, Ming Wang, Stephen C. Boos. Validation of the PediBIRN-7 clinical prediction rule for pediatric abusive head trauma. Child Abuse & Neglect,2024;152:106799.
Disclaimer | Linking Policy | Acceptable Usage Policy | Terms & Conditions (Privacy Policy)
(c) 2021 PediBIRN. All rights reserved. Website and programming by www.WebForMDs.com